Craniosacral
therapy is a gentle hands-on alternative medicine procedure for
evaluating and enhancing the functioning of the craniosacral system, a
physiological system surrounding the brain and spinal cord.
Therapy advocates believe that this system
influences the whole body by affecting the brain and spinal cord, as
well as the brain’s pituitary and pineal gland. As such, the
craniosacral system serves as a core function in that the entire
body’s health depends on its well being. As a core function, the
therapy has the ability to treat a wide-range of disorders and physical
disability, including spinal cord injury ( SCI).
History:
Craniosacral therapy evolved from osteopathic
medicine with its m usculoskeletal emphasis. In the early 1900s,
osteopathic physician William Sutherland concluded that skull bones are
not firmly fixed but can move relative to each other. With these
observations, he developed a treatment called cranial
osteo. In recent years, Dr. John
Uplefurther
developed Sutherland’s observations and incorporated them into a
treatment now called craniosacral therapy.
usculoskeletal emphasis. In the early 1900s,
osteopathic physician William Sutherland concluded that skull bones are
not firmly fixed but can move relative to each other. With these
observations, he developed a treatment called cranial
osteo. In recent years, Dr. John
Uplefurther
developed Sutherland’s observations and incorporated them into a
treatment now called craniosacral therapy.
Dr. Upledger’s interest was whetted early in his
career. While assisting a neurosurgeon in the removal of plaque from a
patient’s spinal cord membrane, Upledger observed the membrane
pulsating in spite of his best efforts to keep it still. This was his
first observation of the craniosacral rhythm. He later researched this
phenomenon for eight years as a professor of biomechanics at Michigan
State University (East Lansing). To more effectively transfer his
research findings to consumers, in 1985, he established the Upledger
Institute in Palm Beach Gardens, Fla. Since then, more than 38,000
practitioners have been trained in craniosacral therapy, including
osteopaths, medical doctors, chiropractors, psychologists, dentists,
physical therapists, acupuncturists, and massage therapists.
The
Craniosacral System:
The spinal cord is surrounded by a protective,
three-layered membrane system (the meninges) that lies within the
vertebral column. The outside layer is called the dura
mater; the middle layer the arachnoid
membrane; and the innermost layer the pia
mater. The inside layer is tightly attached to the spinal cord,
while cerebrospinal fluid is between the other sections.
In addition to providing nutrients, the lubricating cerebrospinal
fluid allows the membrane layers to glide in relationship to one another
as the spine bends and twists. The tough dura mater protects everything
inside of it, including the brain and spinal cord.
The craniosacral system consists of this membrane
system, the enclosed cerebrospinal fluid, the physiological structures
that control fluid input and outflow, and related bones. 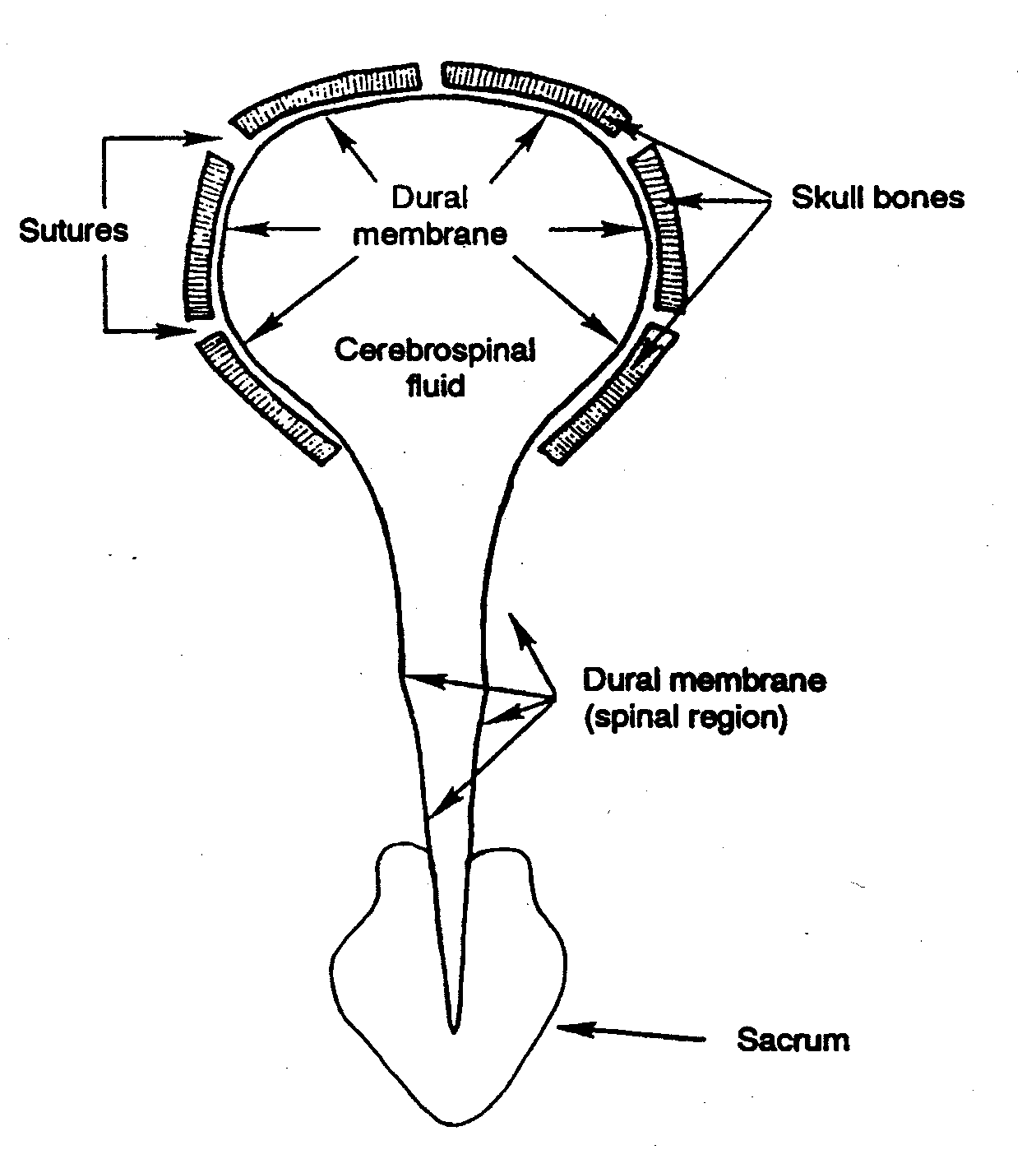 It
is a semi-enclosed biological hydraulic system encompassing the brain
and spinal cord. Within the system, the cerebrospinal fluid rhythmically
pulses at a rate of about ten cycles per minute. This is independent of
heart or respiratory rhythms.
It
is a semi-enclosed biological hydraulic system encompassing the brain
and spinal cord. Within the system, the cerebrospinal fluid rhythmically
pulses at a rate of about ten cycles per minute. This is independent of
heart or respiratory rhythms.
The craniosacral system’s fluid barrier is the
dura mater, which also composes the skull’s inside lining. Dr.
Upledger’s research indicates that the skull bones must be slightly
moving continuously to accommodate the fluid pressure changes within
this semi-closed hydraulic system. The membrane barrier is also attached
to the upper neck vertebrae, the lower back sacrum, the tailbone, and
the openings in the spinal column where nerves go out to the body.
Any occurrence that interferes with the
membrane’s ability to accommodate the rhythmically fluctuating fluid
pressures and volumes is a potential problem.
Craniosacral therapy’s object is to find areas of
restricted movement that compromise function and re-establish normal
movement. Because the craniosacral system encloses the brain and spinal
cord, it influences the entire nervous system, affecting many body
functions. These include the brain’s important pituitary and pineal
glands. These glands, in turn, have the potential to affect the body’s
entire hormonal balance.
The
Controversy:
Mainstream medicine has criticized craniosacral
therapy, sometimes vociferously, primarily because the underlying theory
challenges many classical anatomical assumptions. For example, Dr.
Stephen Barrett (www.quackwatch.com),
an outspoken alternative medicinet critic, says
“the theory behind craniosacral therapy is erroneous because
the bones of the skull fuse during infancy and cerebrospinal fluid does
not have a palpable rhythm.”
Dr.
Rosenfeld’s Guide to Alternative Medicine echoes the former
concern. However, this dogma is not universally accepted. In parts of
Europe, for example, it is taught that the skull bones do, indeed, have
movement potential.
Dr. Upledger feels that the axiom about fused skull
bones may have come from the routine practice of using for anatomical
examinations, long-time-after-death cadavers treated with preservative
chemicals. He says that fresh, unpreserved sutures (the skull bone
edges) are full of dynamic tissue, nerves, and blood vessels, consistent
with a flexible system allowing some movement.
In contrast, the sutures from old preserved skulls appear
calcified.
Dr. Upledger says most neurosurgeons have not
observed the craniosacral rhythm because most surgery penetrates the
membrane barrier required to maintain the rhythm.
In his guide, Dr. Rosenfeld basically agrees, noting
“Unfortunately, none of my colleagues… among others, some very good
neurologists - has ever seen, touched or had any other contact with
cerebrospinal fluid except after withdrawing it for analysis.”
A Hands-on
Process:
During craniosacral therapy, trained therapists use
a light touch equivalent to a nickel’s weight, and feel the rhythmic
motion of the cerebrospinal fluid within the craniosacral system.
Therapists check the rate, amplitude, symmetry, and quality of this
wave-like motion in places where the craniosacral membrane barrier
attaches to bones such as the skull, sacrum and tailbone. Any
restrictions or blockages are treated with light-touch adjustments.
A restriction in one part of the craniosacral
system can affect the entire system, so treatment may involve working at
a point distant from the overt symptom. By assisting the hydraulic
forces in the craniosacral system and, in turn, improving central
nervous system (CNS) functioning, treatment facilitates the body’s
innate, self-healing mechanisms.
Spinal Cord
Dysfunction:
The Upledger Institute’s Brain and Spinal Cord
Dysfunction Program treats about 120 people each year. Most reportedly
have some improvement, ranging from modest to fairly dramatic. Change
takes place with motor function, bowel and bladder control, spasticity
management, and overall well being and ease.
Because patients are usually at least 2-3 years post injury,
improvement is not attributed to residual, ongoing functional
improvement often observed in the first year after spinal cord injury.
The facility customizes the intensive, two-week
program to the person. It may include a variety of additional hands-on
therapies, such as massage, acupuncture, and a craniosacral-related
therapy called somatoemotional
release. In part, these procedures are designed to help muscles that
are spastic, injured, hypertonic or unused; they also help energy flow
and balance. Individuals are usually treated once a year, often with
some follow-up therapy at home. Each day starts with a group discussion
that includes patients and therapists, followed by two hours of hands-on
therapy in the morning and afternoon.
As in the case of many health-care professionals
using substantial hands-on, bodywork, experienced craniosacral
therapists feel as if they can “read” the body.
For example, they can localize the level of injury without other
information. Furthermore, they often note the presence of secondary and
tertiary injury sites resulting from the mechanics and vector forces of
impact. A C-4 quadriplegic, for example, may have experienced secondary
trauma at the T-5 level.
Dr. Upledger says initial trauma results in edema.
A burst of cerebrospinal fluid results in tissue separation that heals
with fibrous scarring. “It is like a copper wire after being hit with
a hammer; it won’t conduct as well,” he says.
Because this secondary damage occurs relatively
soon after injury, Upledger believes that to get fluids moving, patients
should receive treatment within the first month after injuries.
Unfortunately, under the current standards of medical care, access to
craniosacral therapy would be unlikely.
Jackie, who has received therapy in the program,
was injured in a 1990 car accident and is an incomplete quadriplegic. He
has been treated several times at the facility beginning last year and
emphatically states that “they have helped me more than anyone ever
has before. I now have much
more feeling and muscle control.” Jackie now walks without the full
leg brace that was previously needed.
He is a man that likes to “work hard and play
hard,” and his improved trunk muscles, critical for balance, allow him
to use a three-wheel motorcycle once again. He distinctly remembers the
moment on the therapy table that he first regained some feeling in his
left hip. “The tingle felt like the sensation when you try to move a
leg that has gone to sleep.” Jackie says patients and staff develop
tremendous rapport. “They
are like your next-door neighbors.”
As is the case for many treatments, alternative and
mainstream, scientifically rigorous clinical studies have not supported
craniosacral therapy for spinal cord injury and dysfunction.. Although
results appear promising, they are still only anecdotal. However, given
the growing base of these anecdotal results and evidence supporting the
existence of a craniosacral system, the therapy’s potential appears
promising for many.
Contact: The
Upledger Institute at 561/622-4334 or http://upledger.com.
Adapted from an article appearing in the November
1998 issue of Paraplegia News (For
subscriptions, contact www.pn-magazine.com).