Acupuncture, a key element of Traditional Chinese
Medicine, has become a widely popular alternative medicine with the
American public in recent years. This treatment has considerable
potential for treating problems associated with physical disability,
including spinal cord injury (SCI) and
multiple sclerosis. Acupuncture’s potential includes the intriguing
possibility of restored function.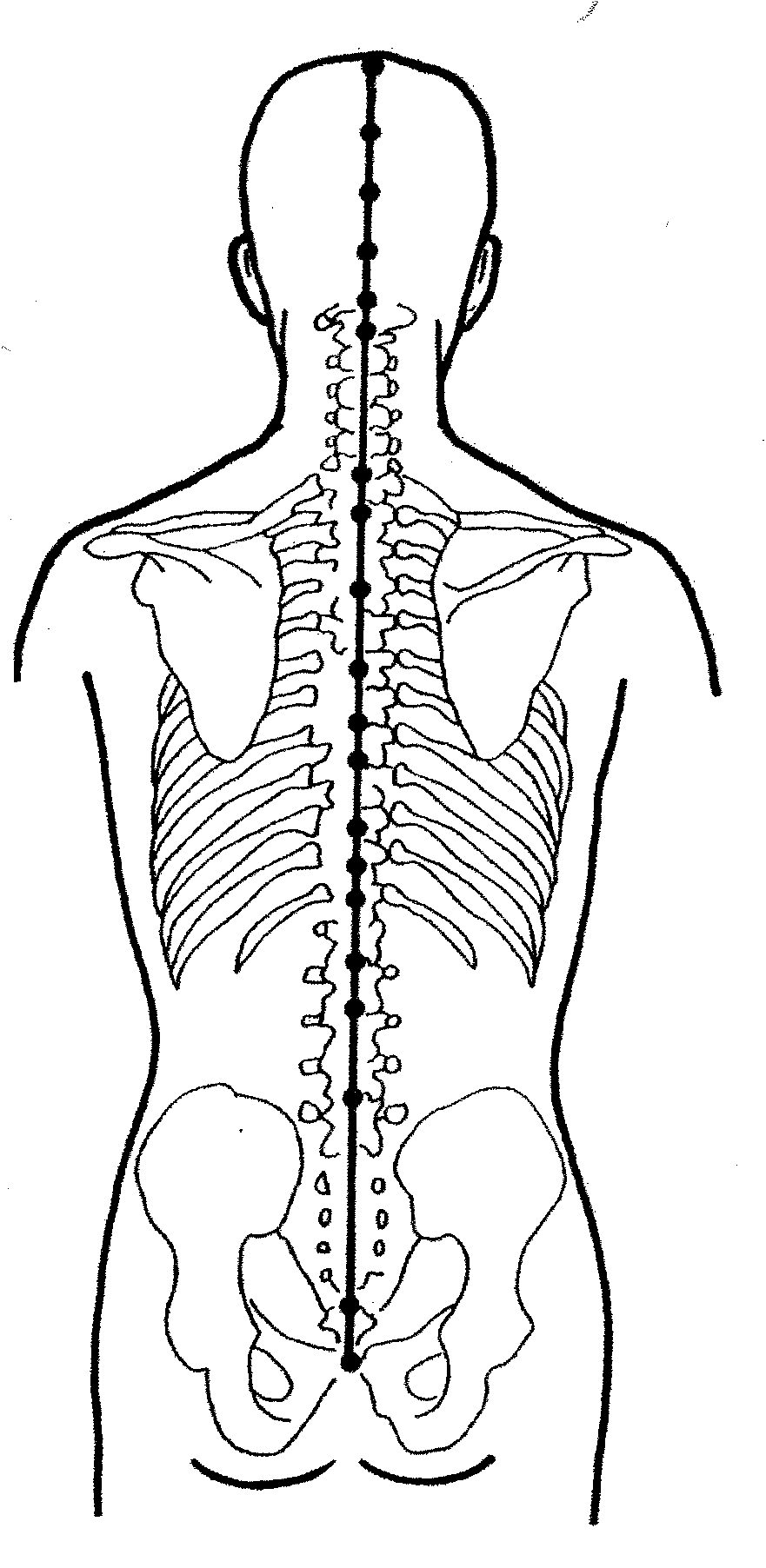
History
Although acupuncture has a 5,000-year tradition,
the transition to the west has been slow. Sixteenth century Jesuit
missionaries first reported the procedure. Troops from far-east military
invasions brought the procedure back to France in the 1800s. In 1825,
Benjamin Franklin’s great-grandson translated French work on
acupuncture. However, after a flurry of interest, acupuncture receded
into oblivion in the United States until President Nixon went to China
in the early 1970s. Soon after Nixon’s visit, the American Medical
Association (AMA) pressured the Food and Drug Administration (FDA) to
ban acupuncture needles unless used in an investigation. In turn, the
ban provided the justification to deny health-insurance coverage.
Nevertheless, acupuncture’s popularity grew.
In spite of technically violating federal law, many states
authorized its use, and schools and accrediting organizations were
established. In 1996, after a million Americans used the procedure every
year, FDA finally reclassified acupuncture needles, and insurance began
to covered the treatment. Last year, a prestigious National Institutes
of Health (NIH) Consensus Conference endorsed specific acupuncture
applications.
Treatment
and Diagnosis:
Acupuncture-related therapies consist of
stimulating specific points on the skin by inserting needles or applying
heat, pressure, or massage. Acupuncture
usually is combined with a variety of other Eastern therapies, such as
herbal treatments, food and nutrition therapy, exercise, and meditation. The thin, usually disposable, needles rarely draw blood, and
any discomfort is mild.
The World Health Organization (WHO) has listed over
100 disorders that may be amenable to acupuncture treatment, including
respiratory, eye, mouth gastrointestinal, neurological, orthopedic,
bronchopulmonary, reproductive, hypertension, insomnia, skin, arthritic,
allergic, and addictive disorders. It is rarely used to treat infectious
disease. Acupuncture seems to work better at early stages before
impaired body function progresses into organic or tissue damage. It is
often a preventive measure to preserve good health. Adverse reactions
are rare, especially compared to drugs or other medical treatments.
Acupuncture emphasizes diagnosis. The Western name
for a disorder (for example, asthma) has little diagnostic relevance.
Two patients with the identical disorder may receive very different
treatments according to their specific energy imbalances. Diagnostic
methods include patient observation, history taking, and touch.
Examining the tongue and feeling the pulse are especially important.
Evaluating the pulse is much more involved than in
Western medicine. A yin and yang pulse is at three locations on each
wrist, measured by deep and light-touch pressure. Each of these 12
different pulses corresponds to a specific organ. When the pulse of both
wrists are taken simultaneously, the relative differences indicate the
body’s energy balance with respect to specific organs.
Although both medical doctors (MDs) and non-MDs can
practice acupuncture, non-physician practitioners usually have had much
more extensive training. Physicians
can pefrorm acupuncture after 200 hours of training; non-MDs must train
over three years in an accredited school of oriental medicine.
Dr. Claire Cassidy, of the Traditional Acupuncture
Institute in Columbia, Md., recently surveyed approximately 600
Chinese-medicine patients from six U.S. clinics. According to her
study’s data, acupuncture appears to be doing something right compared
to Western medicine. This survey indicated that 87% of the people who used
acupuncture and oriental medicine were very satisfied with their care,
91% with their practitioner, 70% were happy with the cost, and 91%
report that their presenting problem has improved. In comparison, only
30 % were satisfied with conventional biomedical care, 43% satisfied
with their physician, and 26% satisfied with the price.
Eastern
Origins:
With
origins in Taoist philosophy, acupuncture evolved from observing that a
disorder was associated with an increased sensitivity in specific areas
of skin. These were consistently linked to a specific organ and followed
a defined topographical pattern. These
patterns or meridians serve as
pathways for life-force energy called qi (pronounced chee). The body is
endowed at birth with a fixed amount of qi which is then depleted
through activities of daily living and supplemented by energy obtained
from food or air. Energy imbalance, whether excessive or lacking, is the
cause of all illness; the absence of qi is death. qi circulates
throughout the body in a well-defined cycle, moving from meridian to
meridian and from organ to organ.
Qi is characterized by the dynamic interaction of
two antagonistic, yet complimentary energy forces called yin
and yang, each of which includes a portion of the other (see
figure). Yin, the feminine, is associated with cold, dark, passive, and
that which is deep or hidden. In contrast, yang, the masculine,
represents heat, light, active, and that which is on the surface. Yin
and Yang are constantly interacting and changing, and one never exists
in isolation from the other.
According to Chinese tradition, all substances are
formed from fire, water, earth, metal, and wood. Fire contains the most
yang and water the most yin. The elements are created or destroyed by
specific cyclical interactions. For example, fire melts metal, metal
cuts down wood, wood covers earth, earth absorbs water, and water puts
out fire.
To each element is assigned one yin and one yang
organ. Under this model, a bad heart (a fire organ) will adversely
affect the lungs (a metal organ), which will in turn affect the liver
(wood). Each organ has a meridian associated with it containing a series
of acupuncture points. Stimulating these points regulates energy flow in
the meridians. Overall, it is a closed system in which the excess of
energy in one area reduces the energy in another area.
Eastern medicine is interactive and holistic -
everything affects everything. In contrast, western medicine emphasizes
component parts (e.g., kidney) without seeing a relationship to the
whole. The focus is on the symptoms, which according to Eastern medicine
are merely the “footprints” left by energy imbalances.
Scientific
Basis:
Although the theory behind acupuncture is based on
centuries of empirical, clinical observations, it was developed without
the benefit of modern physiological and anatomical insights. Because the
idea of an intangible life-force qi flowing through anatomically
undefined meridians seemed far-fetched to those trained in western
medicine, it was dismissed for many years.
Any effects were often attributed to heightened suggestibility,
although the critics could not explain how such suggestibility would
work in animals and young children.
Scientists have now proposed a number of
physiological mechanisms for acupuncture:
·
The procedure stimulates neural pathways and mediates a
variety of neurotransmitter systems. For example, acupuncture has been
shown to stimulate muscle sensory nerves, which send messages to the
spinal cord, midbrain, and pituitary. This stimulation releases
pain-reducing molecules called endorphins
and cortisol-producing hormones that help conditions such as arthritis.
·
Acupuncture points often correspond to skin areas with
unique anatomical and electrical properties.
·
Through the release of specific molecules, it appears that
acupuncture can dilate blood vessels, thereby improving circulation.
Since Eastern medicine assumes that physiological
and molecular alterations are based on changes in energy flow, are
acupuncture-induced hormonal and neurotransmitter changes secondary to a
still scientifically undefined “qi” mechanism? Some investigators
now believe this is so. They propose that the body’s qi energy may
correspond to very subtle bioelectromagnetic fields.
Acupuncture perturbs these fields; the perturbation is then
magnified through more traditional physiological mechanisms.
Most living systems are sensitive to such low fields.
The contribution of these fields to our biological understanding
has been minimal due to difficulties measuring them and the traditional
emphasis on molecular mechanisms.
Some people suggest that integrating molecular and
energy-field approaches would greatly reduce the division between
Eastern and Western medicine. Like yin and yang, harmoniously
integrating Eastern and Western medicine may represent a more balanced
approach to health care.
Clinical
Trials:
A key difficulty in proving acupuncture’s
effectiveness is the FDA requirement to use double-blind, randomized
clinical trials. In such a trial, neither the patient nor doctor knows
who is receiving treatment as opposed to a placebo control. Although
these trials generally work well for drugs, they do not for acupuncture.
As a placebo control, many clinical studies
attempted to insert needles in “sham” acupuncture points (i.e.,
wrong points). Because the results of such studies were ambiguous at
best, they reinforced the skeptics. However, these studies were
fundamentally flawed for a number of reasons.
A major one was that the sham acupuncture points were not neutral
controls. Although not as
effective as true acupuncture points, sham points also evoked a
physiological response.
Overall, criticism leveled at acupuncture should be
placed within the context of the following NIH Consensus Conference
statement: “While it is often thought that there is substantial
research evidence to support conventional medical practices, this is
frequently not the case…the data in support of acupuncture are as
strong as those for many accepted western medical therapies.”
Acupuncture
& Spinal Cord Dysfunction:
People with spinal cord dysfunction can benefit
from most acupuncture applications just as readily as able-bodied
individuals can. Given the health problems common to those with spinal
cord dysfunction, some of these applications may provide a valuable
treatment option in addition to more conventional approaches, such as
drugs.
SCI
Evidence suggests that acupuncture has the
potential to restore some function in both acute and chronic SCI.
Virtually all chronic injuries have some intact, but dormant, neurons
running through the injury site. Acupuncture may work by somehow turning
on these dormant neurons. Animal studies suggest that only a small
percentage of turned-on neurons are needed to have significant function.
The number of published studies focused on
acupuncture’s SCI benefits has grown considerably in recent years;
several are summarized below
Anecdotal Stories
Artie’s First Session:
Artie, a combat-injured Vietnam veteran, was treated by acupuncturist
Kelly for the first time. As is the case with many long-time wheelchairs
users, Artie had chronic, overuse problems with his shoulders and other
areas. Although a wheelchair, who had recently ridden across Vietnam in a
hand cycle, he was, nevertheless, initially apprehensive.
Artie noted, “After years of
being treated and analyzed by detached medical professionals, I was amazed
how relaxed I quickly became. Kelly had a gentle, soothing style with an
intuitive appreciation and understanding of the body. I didn’t have to
tell her; she quickly identified my sore-point areas. Furthermore, I was
surprised that half the time, I didn’t even know that the needles had been
inserted. That night, my bad arm had no pain; I didn’t even have to take
my usual pills.”
Jim’s Story: “I am a
49-year old Vietnam veteran. Due to depression resulting from
post-traumatic stress combined with overmedication, I attempted suicide. I
stuck a gun to my chest and shot myself. The bullet missed my heart and
deflected off my sternum into my spine. My discharge summary reads T-12
SCI, permanent paralysis.”
“After attending a wedding in
Bolivia, I hooked up with a South Korean acupuncturist. I ended up having
30 days of inexpensive treatment and continued it back home. The speed at
which I am rehabilitating is overpowering. Two weeks ago, I walked on a
treadmill for almost two minutes (kafo on left leg and plastic afo on
right leg). Presently, I can walk 45 feet with the kafo unlocked assisted
by a rolling walker. The improvement I have gained is a direct result of
my acupuncture treatments.”
MS
Dr. Naeser (Journal
of Alternative and Complementary Medicine,Vol. 2, 1996, pp.211-248)
has summarized the results of various acupuncture studies involving the
treatment central nervous system paralysis, including spinal cord injury
and multiple sclerosis (MS). The SCI studies basically parallel the
results reported above. For MS, the studies, involving 42 people,
indicated that acupuncture improved muscle spasms, vision, sleep, sexual
functioning, and bladder control. In one case, a woman, who had not been
able to walk unassisted in 15 years, was able to walk unaided 100 feet
after one-year of treatment.
Also, check out the article on
acupuncture and MS.

In conclusion, acupuncture has considerable
potential to treat health problems associated with spinal cord
dysfunction and in some cases, restore significant,
quality-of-life-enhancing function.
For further information, including practitioners in
your area: www.qi-journal.com
and www.acupuncture.com.