This ongoing “Healing Options” series has
periodically discussed various, commonly consumed substances, which may
provide some neuroprotection when administered soon after spinal cord
injury (SCI). Examples include the cholesterol-lowering statin
drugs (e.g., Lipitor), painkiller ibuprofen, herbal remedy
Ginkgo biloba, sleep-inducing hormone melatonin,
cancer-fighting quercetin found in foods, and the ubiquitous
supplement vitamin E. This update specifically discusses another
potential neuroprotectant with extensive human use, specifically the
hormone estrogen.
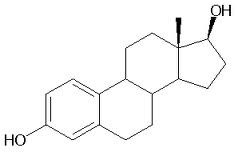
Estrogen
Although estrogen exerts many physiological effects
in both women and men, it is most well known as the female sex hormone.
In women, estrogen is primarily produced by the ovaries. It regulates
the female estrous or reproductive cycle, and promotes the development
of secondary sexual characteristics.
In men the hormone is produced at a much lower
level by the testis, and plays a key role in testicular function. In
aging men, elevated estrogen levels are associated with an increased
risk of stroke, heart disease, and prostate problems, and low levels
with osteoporosis and bone fractures.
Estrogen derivatives are a key component of many
oral contraceptives and have been used for postmenopausal
hormone-replacement therapy. Although estrogen’s reproductive roles
receive the most attention, this potent, multiactive hormone can
influence diverse physiological processes. As such, it theoretically has
broad therapeutic potential much beyond its more obvious roles,
including as a possible protective agent after neurotrauma.
Estrogen & SCI
The SCI neuroprotective possibilities have been
extensively studied by Dr. Naren Banik and colleagues at the Medical
University of South Carolina using animal models of SCI, as well as
cultures of neuronal cells.
_small.jpg)
Animal Studies: SCI was produced by
accessing the thoracic spinal cord of rats through laminectomy and
dropping a weight on the exposed cord. Essentially, this is an
experimental version of the sort of contusion injury experienced by many
individuals with SCI. The rats were then treated intravenously with
estrogen 15 minutes and 24 hours after injury, and, for the next five
days, with a single daily dose injected into the body cavity. Recovery
of locomotor function was followed for six weeks, and the amount of
improvement observed compared to similarly injured control rats which
received no estrogen.
Locomotion was assessed using the BBB scale, a
commonly used animal test which measures recovery of
hind-limb function on a scale from 0 (no hind-limb movement) to 21
(normal walking). At the end of the observation period, the average BBB
score for the estrogen-treated rats was 13 compared to nine for the
controls. Functionally, these statistically significant differences mean
that when compared to controls, the estrogen-treated rats were better
able to support their body weight, make weight-supported steps, and
coordinate hindlimb/forelimb stepping. The investigators concluded that
“estrogen treatment significantly increased the locomotor function in
the injured animals over the 42-day postinjury period…”
Possible Mechanisms: These investigators and
others have devoted much effort trying to understand the specific
biological mechanisms by which estrogen mediates neuroprotection. The
damage-spreading, pathophysiological cascade after the initial physical
insult is extraordinarily complex and is the reason why SCI has been
difficult to understand at a molecular level. Given this complexity, as
well as estrogen’s increasingly documented, powerful multifaceted role
in the body, there are many possible biological systems in which the
hormone could target. Some possibilities are briefly highlighted below.
It is emphasized, however, that these are often complex interlinked and
interdependent processes.
1) Calcium Influx:
Neuronal conduction depends upon the right balance of calcium ions
between the cell inside and outside. Normally, there is a lot of calcium
outside of the neuron and relatively little inside. Injury disrupts the
equilibrium, allowing excessive calcium to flow into the cell. This
influx initiates a neural-destructive cascade that damages other
neurons. By inhibiting the calcium influx into the cells, estrogen
lessens this damaging-perpetuating cascade.
2) Apoptosis:
Cells at the injury site die of necrosis, while cells surrounding the
site often die from apoptosis,. As a crude analogy, necrotic cell death
is like a quick death from being shot and apoptotic cell death is more
like a lingering death from cancer. Because apoptosis is potentially
reversible, treatments that turn this process around should help
minimize postinjury cell degeneration. By modulating the activity of
certain enzymes that promote postinjury apoptosis, estrogen slows down
degeneration.
3) Excitotoxicity:
Routinely, certain amino acids, like glutamate, are released from a
pre-synaptic neuron and flow to a nearby post-synaptic neuron,
promulgating the nerve impulse. However, after injury, cells burst,
releasing too much glutamate. Through interactions with receptors on
neighboring cells, this excessive glutamate will initiate a neurotoxic
biochemical cascade. Estrogen protects against this
excitotoxicity-caused cell death.
4) Edema: Fluid
accumulation at the injury site creates damaging edema swelling.
Estrogen-treated rats exhibit less edema.
5) Inflammation:
Inflammatory cells infiltrate into the lesion area, which promotes
secondary cell death. Estrogen treatment lessens infiltration.
6) Myelin: The
fatty insulation surrounding axons, myelin enables neurons to propagate
a signal. SCI often results in axonal demyelination, another process
which is attenuated by estrogen.
7) Blood Flow:
Injury compromises regeneration-promoting blood flow, contributing to
secondary cell death. Estrogen promotes the growth of new blood vessels
(i.e. angiogenesis), enhancing postinjury blood flow.
8) Antioxidant:
After the initial mechanical injury in SCI,
free-radicals are generated. Called lipid peroxidation, these free
radicals can steal electrons from neighboring cell membranes, resulting
in further cell death. A potent antioxidant, estrogen may reduce
free-radical-induced oxidative stress.
Given these findings and the fact that women have
much higher levels of estrogen than men, it is interesting to note that
studies suggest that women recover more function after neurotrauma.
Need for New Treatment Options
Before you grab your wife’s birth-control pills,
remember estrogen’s promising neuroprotective potential is based on
animal studies often using high dosing, which doesn’t necessarily
translate into human efficacy. Nevertheless, we clearly need to develop
new SCI-treatment options. Since the 1990s, the big tamale for
treating acute injury has been high-dose methylprednisolone (MP), a
synthetic glucocorticoid steroid. Unfortunately, this therapeutic tamale
is causing heartburn for a growing number of scientists.
Although several large clinical trials sponsored by
the National Institutes of Health suggested that MP preserves function,
more recent studies are questioning these conclusions. For example,
emerging research suggests that high-dose MP therapy damages muscles and
that functional improvement attributed to MP may merely be due to the
recovery of muscle damage caused by the drug itself. In addition, a
recent Japanese study indicates that MP-treated patients actually had
less improvement than non-MP-treated patients.
Because MP was so wholeheartedly
embraced by SCI-health policymakers, the consideration of other options
was regrettably pushed to the backburner. Although we could argue
endlessly on MP’s true therapeutic value, it certainly won’t hurt to
expand our SCI-healing armamentarium through a renewed focus on
potential alternatives. Although the neuroprotective potential of
estrogen and the substances listed previously have been explored mostly
in animals, their widespread human consumption and the physiological
understandings gained from such consumption give them a leg up in the
translation into real-world therapies.
Adapted from article appearing in
April 2011 Paraplegia News (For subscriptions,
call 602-224-0500) or go to
www.pn-magazine.com.
TOP