A common consequence of SCI is erectile dysfunction
(ED), defined by the National Institutes of Health as the inability to
achieve or maintain an erection sufficient for satisfactory sexual
intercourse. Many approaches of varying effectiveness have been used to
address SCI-associated ED. The purpose of this update is to summarize
some of the approaches and the research supporting their use.

Reflex versus Psychogenic
Erection
The neurophysiology behind erectile functioning is
complex. Basically, there are reflex (produced by physical stimulation)
and psychogenic (mentally induced) erections, each controlled by
different nerve pathways and is affected differently by injury level.
The ability to generate reflex erections depends on
the preservation of neural circuitry in the lower, sacral (S2-4)
spinal-cord segments. Hence, although there is less overall paralysis
from a sacral than a high-level injury, reflex-erection potential will
be more compromised. In contrast, the required sacral neural circuitry
is undamaged in higher injuries, preserving reflex-erection potential.
Psychogenic erections are mediated, in part,
through the thoracic T-10 to lumbar L-2 spinal regions. Hence,
individuals with injuries above this level have lost the ability to
generate psychogenic erections but have maintained reflex-erection
capacity. In contrast, although unable to produce a reflex erection,
those with a sacral injury have the neural pathways necessary to mediate
a psychogenic erection. Men with injuries between the T10- L2 and S2-4
levels may retain both psychogenic and reflex erections.
This situation is confounded with incomplete
injuries in which some function-controlling neurons still cross the
injury site.
Erection Physiology
An erection develops when cylindrical, sponge-like
regions surrounding the penis become filled with blood. Penile
tumescence is initiated by nerve branches releasing a key
neurotransmitter called nitric oxide, which causes penile arteries to
dilate, filling the sponge-like cavities with blood. This process is
mediated by the nitric-oxide-stimulated production of a secondary
messenger molecule called cGMP (cyclic guanosine monophosphate). This
molecule is especially important because Viagra-like drugs inhibit its
degradation, letting it accumulate and, in turn, promoting erection. So
to speak, it is like disabling the brakes on a cGMP-fueled car.
Oral Medications
Sildenafil (Viagra)
As mentioned above, Viagra inhibits cGMP
degradation, therefore, shifting the physiological balance more toward
erection maintenance.
 Numerous
studies have documented Viagra’s SCI benefits for men with SCI:
Numerous
studies have documented Viagra’s SCI benefits for men with SCI:
1) Dr. M. Maytom (UK) et al carried out a
two-part pilot study in men with SCI-related ED. In part 1, 27 subjects
(age 18-55, sustaining injuries at least 1/2 years earlier) received
either Viagra or placebo. After a three-day washout period, the
treatments were reversed. Sixty-five percent had erections sufficient
for penetration after taking the drug compared with only 8% for the
placebo. In Part 2, subjects were randomized to receive either Viagra or
placebo over a 28-day period. Based on questionnaires, 75% and 8% of the
Viagra- and placebo-treated patients, respectively, indicated that
treatment had improved their erections.
2) Dr. F. Giuliano (France) and colleagues
examined Viagra’s effects on 178 men with SCI, who were injured at least
six months before study recruitment. The subjects received either Viagra
or a placebo before sexual activity for six weeks. After a two-week
washout period, treatments were reversed. Evaluated by patient
questionnaires and feedback, 80% reported that Viagra improved sexual
intercourse compared with only 10% for placebo. The most common side
effects were headaches, flushing, and indigestion.
3) Dr. D. M. Schmid and colleagues
(Switzerland) prospectively studied the effects of Viagra in 41 men with
SCI. Ninety-three percent responded positively to Viagra, obtaining a
sufficiently rigid erection for sexual intercourse. About 10% had side
effects, such as headaches or dizziness.
4) Drs. B. G. Green and S. Martin (USA)
studied Viagra’s effects in 40 men with spinal cord dysfunction (both
SCI & MS). Followed for up to two years, erectile response improved from
4.9 to 7.8 on a scale of 1-10, and 90% obtained erections sufficient for
intercourse.
5) Dr. A. Sanchez Ramos et al (Spain)
studied Viagra’s safety and efficacy in 170 men with SCI. Assessed by
questionnaires, 88% of the subjects and 85% of their partners reported
improved erections as a result of the drug. The investigators concluded
that Viagra is an “effective, well-tolerated treatment for erectile
dysfunction caused by spinal cord injury, regardless of the cause,
neurological level, ASIA grade, and time since injury.”
6) One of Viagra’s side effects in neurologically
intact men is hypotension or low blood pressure. Because individuals
with higher level SCI are prone to hypotension, Dr. K. D. Ethans
and colleagues, (Canada) studied Viagra’s effects on blood pressure in
men with SCI. Although blood pressure changed little in subjects with
thoracic injuries, it decreased significantly in those with cervical
injuries.
7) Dr. S. Ergin et al (Turkey) studied the
effects of Viagra on 50 men with SCI. Subjects averaged 39 years in age
and had been injured at least six months before recruitment.
Approximately 58% had complete injuries. The subjects were randomized to
receive either Viagra or placebo for six weeks. This was followed by a
two-week washout period and then treatment reversal. Based on subject
feedback, the investigators concluded that Viagra “produced higher
levels of successful stimulation, intercourse success, satisfaction with
sexual life and sexual relationship, erectile function, overall sexual
satisfaction…”
Vardenafil (Levitra)
Levitra is in the same drug class as Viagra and
promotes erectile potential through similar physiological mechanisms.
Dr. F. Giuliano et al (France) evaluated the
effectiveness and tolerability of Levitra in 418 men with SCI sustained
at least six months before study enrollment. Subjects were randomized
to receive either Levitra or a placebo. Erectile function was measured
by questionnaires and diary questions concerning penetration, erection
maintenance, and ejaculation. All of these measures improved in the
Levitra-treated group. Side effects reported most often included
headache, flushing of the skin, nasal congestion, and stomach pain.
Dr. Y. Kimoto and colleagues (Japan) treated
32 men with SCI with varying Levitra doses. The investigators concluded
that drug was “well tolerated and improved erectile function in patients
with SCI.” Twenty-two percent of patients reported mild and transient
side effects such as hot flushes and headaches.
Tadalafil (Cialis)
Cialis also works in a fashion similar to Viagra or
Levitra. However, unlike these other drugs, whose effectiveness is
limited to about four hours, Cialis will enhance erection potential for
up to 36 hours.
Dr. F. Giuliano (France) and associates
treated 186 subjects with SCI with either varying doses of Cialis or a
placebo. Of these individuals, 69% had complete injuries; 84% had
thoracic, lumbar, or sacral injuries; and 69% had moderate to severe ED.
Eighty-five percent of the Cialis-treated subjects reported improved
erections compared with only 19% for placebo-treated subjects.
Seventy-five percent of the Cialis-treated men were able to penetrate
their partner compared with only 44% before treatment; and 48% reported
successful intercourse compared with only 11% before treatment.
Headaches and urinary tract infections were the most common side
effects.
Dr. G. Lombardi (Italy) and co-investigators
followed 65 men with SCI who had been taking Cialis an average of nearly
34 months. They reported a significant improvement in erectile function,
sexual satisfaction, and overall satisfaction and concluded that Cialis
“represents an effective and safe long-term option for SCI patients with
ED.”
Intracavernosal Injection
Erectile tumescence occurs when cylindrical,
sponge-like regions on each side of (corpus cavernosa) and below the
penis shaft become engorged with blood. Injection of certain agents into
the cavernous regions consistently produces erections in men with
SCI-related ED. Basically, these substances enhance erection-promoting
blood flow into the penis. An occasional side effect is priapism, a
prolonged erection, in which the penis does not return to its flaccid
state within about four hours. Penile scaring is also possible at the
site of injection.

Alprostadil is identical to natural occurring
prostaglandin E1 (PGE1). Prostaglandins are found in most
tissues and hormonally exert many physiological effects. Alprostadil
intracavernosal injections are marketed under various brand names,
including Caverject. Other substances used for SCI-related ED include
papaverine, a non-narcotic opiate; phentolamine, a drug used to treat
adrenal-gland tumors; and atropine.
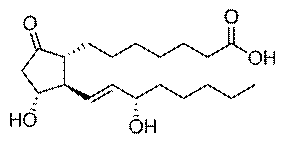
Alprostadil or Prostaglandin E1
Several studies have been carried out evaluating
the use of intracavernous injections to treat SCI-related ED:
Dr. G. Beretta et al (Italy) treated 22 men
with SCI with intracavernous injections of papaverine, of whom 20
obtained complete penile rigidity. Seven had erections lasting more than
300 minutes.
Dr. A. Sidi and colleagues (USA) treated 66
patients with SCI with intracavernous injections containing either
papaverine or a combination of papaverine and phentolamine. All 52
patients who completed the protocol “achieved transient functional
penile erections”; four suffered priapism requiring treatment.
Dr. C. M. Earle et al (Australia) treated 22
men with SCI with various intracavernosal agents, including papaverine,
papaverine plus phentolamine, or PGE1. Nineteen responded to therapy.
Twelve of 14 who participated in a follow-up mail survey continued to
periodically use the drugs and reported satisfaction with their use.
Dr. V. K. Kapoor and colleagues treated 65
men with paraplegia and 36 with quadriplegia with intracavernous
papaverine. Of these, 98 had erections sufficient for penetration, and
three had prolonged erections lasting more than four hours.
Dr. I. H. Hirsch et al (USA) evaluated
intracavernous PGE1 treatment in 27 men with neuropathic erectile
dysfunction (14 with SCI). “Quarterly monitoring up to 28 months
demonstrated satisfactory erectile rigidity and duration of erection.”
No priapism was observed.
Dr. S. Zaslau and colleagues (USA) treated
28 men with intracavernous injections containing a combination of
papaverine and PGE1. Of those who completed the study, 85% indicated
that their erections were good or excellent, and 77% were moderately or
extremely satisfied with treatment. Average erection duration was 43
minutes.
Intraurethral Suppository
Alprostadil can also be administered by inserting a
small medicated pellet in the urethral opening (the passage from the
bladder to the outside through which urine flows). Absorbed by the
urethral tissue, the medicine passes through to the surrounding erectile
tissue. This treatment is marketed by under the name MUSE, an acronym
for “medicated urethral system for erections.”
The method is less invasive and considered easier
for quadriplegics who may lack the hand function needed for
intracavernosal injections. To enhance erectile rigidity, it has been
used with a constrictor band at the base of the penis, which also limits
the systemic absorption of the drug into the rest of the body.
Studies suggest that the treatment is less
effective than injections, and high drug doses were required to produce
sufficient tumescence. For example, Dr. D. H. Bodner and
colleagues (USA) evaluated the ability of MUSE to treat ED in 15
patients with SCI. The investigators concluded: “MUSE appears somewhat
effective in creating erections; however, these were less rigid
erections than those obtained with intracavernosal therapy and provided
less overall satisfaction.”
Topical Agents
A number of less-invasive, but less-effective,
topical agents enhance erectile potential. For example, Topiglan, rubbed
on the penis tip, contains alprostadil together with a substance that
increases skin absorption. Dr. I. Goldstein and colleagues (USA)
randomized 60 men with moderate to severe ED to receive either Topiglan
or a placebo gel. About 40% of those who received the active gel
developed erections sufficient for vaginal penetration compared with
only seven percent of controls. Other studies include:
Drs. J. Sonksen and F. Biering-Sorensen
(Denmark) studied the erection-producing effects of placing
nitroglycerin-containing plasters on the penile shaft of 17 men with SCI
(Nitroglycerine is a vasodilator, i.e., a blood-flow-increasing
substance.) All had responded previously to intracavernous papaverine
injections sufficient for vaginal penetration. A positive response was
obtained in 12 of the men. Five were able to achieve erections
sufficient for vaginal penetration at home and preferred the method over
the previously used injections.
Dr. G. Beretta et al (Italy) examined the
erectile properties of minoxidal (another vasodilatory agent) topically
applied to the penile shaft in 15 men with SCI. Of the four who reported
a positive erectile response, three preferred to continue with this
noninvasive treatment over intracavernous injections.
Drs. E. D. Kim and K. T. McVary (USA)
evaluated the effect of topically applied alprostadil on erection
function in 10 men, nine of whom had SCI. Blood flow in the arteries
serving the erection-producing cavernous tissue increased in seven.
Dr. E. D. Kim and associates (USA) examined
the effects of topically administered papaverine gel in 20 men with ED,
of whom 13 had SCI. The investigators concluded that “papaverine gel
appears to be safe and well tolerated… and increases blood flow to the
penis.” They also noted that the application of the gel to the genitalia
resulted in little systemic absorption and, as a result, less potential
to exert physiological effects in other parts of the body.
Dr. R. Renganathan and colleagues (India)
compared the effectiveness of intracavernous injections of papaverine
with nitroglycerin transdermal patches in treating ED in 28 men with
SCI. Ninety-three percent who received an intracavernous injection of
papaverine demonstrated a complete erectile response compared with only
61% who used the transdermal nitroglycerin.
Vacuum Devices
Vacuum devices have been shown to enhance erections
in men with SCI-related ED. With these devices, a cylinder attached to a
vacuum pump is placed over the penis, and the resulting vacuum draws in
erection-producing blood. A constriction ring is then temporarily placed
around the penis base to maintain the erection. The devices have been
evaluated in a number of SCI-focused studies:
Drs. N. Zazler and P. G. Katz (USA)
prospectively examined vacuum-device effectiveness in 20 men with
injuries ranging from the C-4 to L-2 level. Subjects ranged in age from
21 to 65 (average 40), had been injured for at least a year, and had a
steady sexual partner. Evaluated by subject and partner questionnaires,
all reported successful intercourse after having used the device at
least 20 times. The majority indicated that intercourse quality was very
good or excellent compared to the previous best since injury. The
investigators concluded the device “was an effective, safe, non-invasive
alternative for the management of impotence secondary to cord injury.”
Dr. L. Heller et al (Israel) studied the use
of such devices in 30 subjects with chronic neurological impotence.
After training at the clinic, 17 chose to use the device at home, and 21
months later, 50% were still using it. Intercourse frequency increased
from 0.3 to 1.5 times a week.
Dr. J. Denil and associates (USA) evaluated
the erection-promoting potential of vacuum devices in 20 men with
SCI-related ED. At three months, 93% of them and 83% of their female
partners reported erection sufficiently rigid for vaginal penetration
(average duration 18 minutes). At six months, 41 and 45% of the men and
women, respectively, were satisfied with the device, with early rigidity
loss the most common complaint.
Implants
Both malleable and inflatable penile implants have
a relatively long history of use for SCI-related ED. With the former,
semi-rigid cylinders are implanted into erectile tissue; the device is
bent outward for sex and back toward the body for concealment. With a
two-piece inflatable device, inflatable cylinders are connected to a
ball-shaped pump locate in the scrotum, which, when squeezed, sends
fluid from the back of the cylinder to its mid-area, producing erectile
rigidity. When the middle of the penile shaft is bent, the fluid returns
to the cylinder base.
The potential adverse effects of these implants
have been discussed by several SCI scientists. For example, Dr. S.
Elliot (Canada) has noted: “Men with SCI experience a much higher
infection rate and erosion rate with these devices when compared to
nonneurological patients…Because these devices are placed in the spongy
tissue of the corpora cavernosal bodies, much of the tissue is
permanently destroyed. This precludes the use of other erection
enhancement techniques….” In another example, Dr. D. Deforge and
colleagues (Canada) stated “Penile implants are very satisfactory for
those who do not have complications, but the serious complication rate
was consistently close to 10%. Furthermore, patients who have an implant
removed are likely to have damage to the penile tissues that would make
them nonresponsive to intracavernous injections or vacuum devices.”
Finally, Dr. D. H. Zerman et al (Germany)
reported the results of following 245 men (197 SCI) with neurological
impairment with ED, who had received implants between 1980 and 1996.
Fifty percent had a semi-rigid device implanted, and the rest inflatable
devices. The investigators concluded “The implantation of a penile
prosthesis is a safe procedure for erectile dysfunction… in
neurologically impaired. Based on technical advances the complication
rates significantly decreased during the years.”
Conclusion
In conclusion, the management of erectile
dysfunction for men with spinal cord injury continues to receive
attention in the medical literature. Since the evolution of the penile
prostheses in the 1970s, a growing number of effective treatments have
emerged. As a result, the potential for erections that are suitable for
sexual intercourse is available for any man, regardless of injury, who
wishes to have an erection and who wishes to be sexually active.
Although the effectiveness of these treatments is well documented, a
rigid erection does not necessarily lead to sexual satisfaction. It is
the combination of physical, emotional and relationship issues that
ultimately lead to a fulfilling sexual experience. It is hoped that
future research in erectile functioning after SCI will also investigate
the interaction between the medical and psychological factors.
Note: The Paralyzed Veterans of America has
published a clinical practice guideline entitled Sexuality and
Reproductive Health in Adults with Spinal Cord Injury. Although
targeting health-care professionals, this informative guideline can be
downloaded at
www.pva.org (click on Research and Education).
Adapted from article appearing in May 2010 Paraplegia News (For subscriptions,
call 602-224-0500) or go to
www.pn-magazine.com.
TOP